Origin of Influenza Viruses and Worldwide Transmission
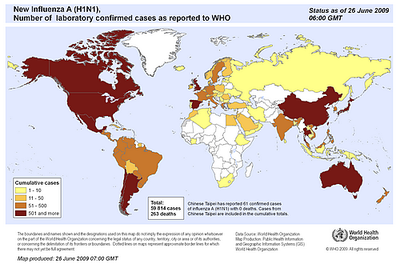
There are descriptions of Influenza in Europe dating back to 1100 A.D., and sporadic, isolated outbreaks have likely been occurring for thousands of years. The term “influenza” was given by an Italian in the mid-1700’s to connote a disease resulting from miasma. The 1918 “Spanish Flu”, rivals the Black Death as the deadliest epidemic in history. With the world already emaciated by war, the 1918 pandemic was devastating; some 30 to 40 million people died globally, with the highest death rate occurring in young men and women. In the United States, 675,000 people died, including over 40,000 G.I.s. Viruses identical or closely related to the human form of the infection can be isolated from ducks, turkeys, swine, horses, and many other species of warm-blooded vertebrates. It is hypothesised that humans acquired influenza when domestication of animals first began. The development of agriculture and the establishment of permanent settlements allowed sufficient numbers of potential hosts to create an epidemic. Wilson Smith, Christopher Andrews, and Patrick Laidrow are said to be the first to identify the virus that causes human influenza because they found a suitable host for propagation.
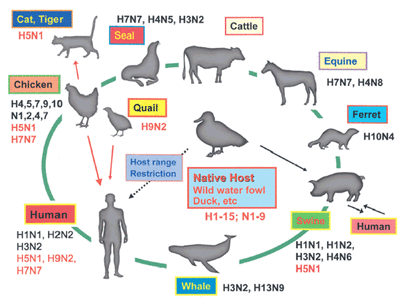
Influenza A viruses are divided into subtypes based on two proteins on the surface of the virus: the hemagglutinin (H) and the neuraminidase (N). There are 17 different hemagglutinin subtypes and 10 different neuraminidase subtypes. All known subtypes of type A viruses have been found among birds, except subtype H17N10 which has only been found in bats. Wild birds are the primary natural reservoir for all subtypes of influenza A viruses and are thought to be the source of influenza A viruses in all other animals. Most influenza viruses cause asymptomatic or mild infection in birds; however, the range of symptoms in birds varies greatly depending on the strain of virus. Infection with certain avian influenza A viruses can cause widespread disease and death among some species of wild and especially domestic birds such as chickens and turkeys.
Pigs can be infected with both human and avian influenza viruses in addition to swine influenza viruses. Infected pigs get symptoms similar to humans, such as a cough, fever and runny nose. Because pigs are susceptible to avian, human and swine influenza viruses, they may potentially be infected with influenza viruses from different species at the same time. If this happens, it is possible for the genes of these viruses to mix and create a new, hybrid, virus. For example, if a pig were infected with a human influenza virus and an avian influenza virus at the same time, the viruses could mix and produce a new virus that had most of the genes from the human virus, but a hemagglutinin and/or neuraminidase from the avian virus. The resulting new virus would likely be able to infect humans and spread from person to person, but it would have surface proteins not previously seen in influenza viruses that infect humans. This type of major change in the influenza A viruses is known as antigenic shift. Antigenic shift results when a new influenza A subtype to which most people have little or no immune protection infects humans. If this new virus causes illness in people and can be transmitted easily from person to person, an influenza pandemic can occur and the disease is spread worldwide.
Flu epidemics spread rapidly and are very difficult to control. Most influenza virus strains are not very infectious and each infected individual will only go on to infect one or two other individuals (the basic reproduction number for influenza is generally around 1.4). However, the generation time for influenza is extremely short: the time from a person becoming infected to when he infects the next person is only two days. The short generation time means that influenza epidemics generally peak at around 2 months and burn out after 3 months. Individuals become infectious before they become symptomatic, therefore putting people in quarantine after they become ill is not an effective public health intervention.
While it is unusual for people to get influenza infections directly from animals, sporadic human infections and outbreaks caused by certain avian influenza A viruses have been reported.
Influenza A viruses are divided into subtypes based on two proteins on the surface of the virus: the hemagglutinin (H) and the neuraminidase (N). There are 17 different hemagglutinin subtypes and 10 different neuraminidase subtypes. All known subtypes of type A viruses have been found among birds, except subtype H17N10 which has only been found in bats. Wild birds are the primary natural reservoir for all subtypes of influenza A viruses and are thought to be the source of influenza A viruses in all other animals. Most influenza viruses cause asymptomatic or mild infection in birds; however, the range of symptoms in birds varies greatly depending on the strain of virus. Infection with certain avian influenza A viruses can cause widespread disease and death among some species of wild and especially domestic birds such as chickens and turkeys.
Pigs can be infected with both human and avian influenza viruses in addition to swine influenza viruses. Infected pigs get symptoms similar to humans, such as a cough, fever and runny nose. Because pigs are susceptible to avian, human and swine influenza viruses, they may potentially be infected with influenza viruses from different species at the same time. If this happens, it is possible for the genes of these viruses to mix and create a new, hybrid, virus. For example, if a pig were infected with a human influenza virus and an avian influenza virus at the same time, the viruses could mix and produce a new virus that had most of the genes from the human virus, but a hemagglutinin and/or neuraminidase from the avian virus. The resulting new virus would likely be able to infect humans and spread from person to person, but it would have surface proteins not previously seen in influenza viruses that infect humans. This type of major change in the influenza A viruses is known as antigenic shift. Antigenic shift results when a new influenza A subtype to which most people have little or no immune protection infects humans. If this new virus causes illness in people and can be transmitted easily from person to person, an influenza pandemic can occur and the disease is spread worldwide.
Flu epidemics spread rapidly and are very difficult to control. Most influenza virus strains are not very infectious and each infected individual will only go on to infect one or two other individuals (the basic reproduction number for influenza is generally around 1.4). However, the generation time for influenza is extremely short: the time from a person becoming infected to when he infects the next person is only two days. The short generation time means that influenza epidemics generally peak at around 2 months and burn out after 3 months. Individuals become infectious before they become symptomatic, therefore putting people in quarantine after they become ill is not an effective public health intervention.
While it is unusual for people to get influenza infections directly from animals, sporadic human infections and outbreaks caused by certain avian influenza A viruses have been reported.